1.Introduction
Nurses constitute the largest group within the hospital workforce, and their role in influencing the quality of healthcare services is crucial. They have extensive daily interactions with patients and, therefore, significantly impact the overall care provided.[1] The efficacy and efficiency of healthcare systems are significantly enhanced by the strong leadership of nurse administrators.[2] Transformational leadership styles have been extensively studied in various professions, including nursing,[3] emerging as particularly effective in enhancing staff outcomes and patient care.
Transformational leadership in healthcare is defined by four key attributes: idealized influence, inspirational motivation, intellectual stimulation, and individualized consideration, which are believed to improve job satisfaction and performance among nurses.[4, 5] This leadership style excels in enhancing communication and team-building, exceeding the transactional model in these dimensions.[6] Transformational leaders are recognized for their capacity to inspire and encourage their teams, fostering psychological safety and trust, essential for enhancing work performance and organizational commitment.[7]
The theoretical foundation for this review draws from Bass and Avolio’s transformational leadership model. Bass (1993)[8] proposed that the transformational leadership construct comprises four sub-dimensions: idealized influence, inspirational motivation, intellectual stimulation, and individualized consideration, which were further refined by Bass and Avolio (1996).[9] The original idea behind transformational leadership was that leaders can appeal to followers’ moral values in order to achieve goals and influence followers to transcend their self-interest for the larger good of their team and organization. In nursing contexts, these four behavioral dimensions are hypothesized to enhance job satisfaction through increased autonomy, support, and professional development, while improving productivity through enhanced motivation and competence development.[10]
Transformational leadership, in contrast to other leadership styles, correlates with elevated job satisfaction and is deemed more appropriate for tackling the intricate challenges confronting contemporary healthcare organizations, including rising patient populations and cost stabilization.[11, 12] While transactional leadership emphasizes exchanges and incentives for achievement, transformational leadership transcends these methods by inspiring followers to exceed their own expectations and contribute beyond their prescribed responsibilities.[7] Ferreira et al.[13] emphasize the importance of transformational leadership styles in enhancing nurse satisfaction, promoting productivity, and improving staff retention and recruitment.
Examining the impact of transformational leadership on nurses’ job satisfaction and productivity is crucial for several reasons. Transformational leadership has consistently shown a positive correlation with increased work satisfaction and decreased turnover intentions among nurses, which is critical because nurse retention is a significant issue for healthcare organizations, and high turnover rates can negatively affect patient care quality and organizational efficiency.[14, 15] Studies demonstrate a connection between transformational leadership and heightened nurse efficiency and involvement.[14, 16] When nurses feel inspired, reinforced, and empowered by their superiors, they are more likely to surpass their responsibilities, ultimately leading to improved effectiveness and patient care quality.
A study conducted in critical care units found that nurses working under transformational leaders reported significantly higher job satisfaction compared to those under transactional leaders, with 23% of the variation in job satisfaction explained by transformational leadership factors such as professional support and intellectual motivation.[17] Additionally, transformational leadership has been linked to improved nurse productivity by promoting communication, personnel development, and service improvement, which are crucial for effective healthcare delivery.[18] The leadership style not only enhances the quality of life for nurses but also reduces turnover rates, thereby contributing to a more stable and efficient workforce.[19]
Despite extensive research on transformational leadership in nursing, systematic synthesis of its effects on job satisfaction and productivity across diverse healthcare contexts remains limited. This gap is particularly significant given increasing globalization of healthcare practices and the need for culturally-informed leadership approaches. There is an urgent requirement for current evidence regarding the implementation of advanced leadership programs for nurse managers in nursing education and practice in countries facing challenges in their healthcare systems.[20, 21, 22]
Previous systematic reviews have focused primarily on Western healthcare contexts or examined limited outcome measures. Our review addresses this gap by synthesizing evidence from multiple countries and healthcare systems, examining both job satisfaction and productivity outcomes to provide comprehensive insights for global nursing practice. By identifying effective leadership approaches, this study aims to provide valuable insights that can strengthen healthcare systems and improve service quality in diverse regions facing similar challenges.
2.Methods
2.1Aim and design
Research Question: What is the relationship between transformational leadership and nursing job satisfaction and productivity across different healthcare settings and cultural contexts?
This systematic review aimed to conduct a comprehensive review and evaluation of quantitative studies that investigate how transformational leadership style impacts the job satisfaction and productivity of nurses in healthcare facilities. This study has the potential to reveal valuable insights that could bring significant enhancements to healthcare management.
This quantitative systematic literature review followed the PRISMA 2020 statement, which is the standard format for reporting the findings of systematic reviews, ensuring clarity and transparency in how the review is presented, and providing a framework for accurately documenting the process and results.[23] We excluded qualitative studies to maintain methodological homogeneity and enable quantitative synthesis of effect sizes. This decision was made a priori to provide robust statistical evidence for transformational leadership effects. The protocol was developed a priori but not registered.
2.2Search strategy
To ensure comprehensive coverage of relevant nursing, medical, healthcare, and multidisciplinary research, the search strategy employed MeSH keywords associated with nurses, transformational leadership, job satisfaction, and productivity. This approach was designed to yield precise and extensive results, capturing a broad set of studies relevant to the topic. The literature search was conducted across five electronic databases from January 2016 to March 2024: PubMed, Scopus, Web of Science, CINAHL, and Google Scholar. The search methodology aimed to identify all relevant quantitative studies that addressed the research problem effectively. Although no geographic filters were applied during the database searches, the review aimed to capture a globally representative dataset, especially including regions underrepresented in earlier systematic reviews (e.g., Middle East, South Asia, and East Asia). The final inclusion of studies was based on methodological criteria and relevance to the review question, not on geographic location. However, the geographic distribution of the included studies—summarized in Table 1—offers insights into how transformational leadership is studied and operationalized across different cultural and healthcare contexts.
| Publication Year | |
| 2016-2018 | 8 (36.4) |
| 2019-2021 | 9 (40.9) |
| 2022-2024 | 5 (22.7) |
| Geographic Distribution | |
| Saudi Arabia | 5 (22.7) |
| Pakistan | 4 (18.2) |
| Jordan | 3 (13.6) |
| Malaysia, Taiwan | 2 each (9.1 each) |
| Indonesia, Egypt, Kuwait, Turkey, Greece, Ethiopia | 1 each (4.5 each) |
| Sample Size | |
| Mean ± SD | 220.3 ± 158.7 |
| Range | 45-719 |
| Total participants | 4,847 |
| Study Design | |
| Cross-sectional | 21 (95.5) |
| Mixed methods | 1 (4.5) (Wang et al., 2021) |
| Primary Instruments | |
| Multifactor Leadership Questionnaire (MLQ) | 17 (77.3) |
| Job Satisfaction Survey (JSS) with MLQ | 8 (36.4) |
| Minnesota Satisfaction Questionnaire (MSQ) | 4 (18.2) |
| Other instruments |
6 (27.3) |
The researchers deconstructed the research question into its PICO components, identified keywords using the PICO framework as outlined in Table 2, found synonyms for the search terms, and combined the keywords and phrases using Boolean operators (OR and AND).
| P (Population) | Nurses |
| I (Intervention) | Transformational Leadership Style |
| C (Comparison) | No intervention/Other leadership styles |
| O (Outcomes) | Job Satisfaction and Productivity |
The search terms specified included “Transformational Leadership”, “Nursing”, “Job Satisfaction”, “Productivity”, “Nurses”, and “Healthcare Facilities”. Synonyms and related phrases were also incorporated, such as pairing the term “Productivity” with “performance”, “nursing”, “nurses”, “Healthcare Facilities”, and “hospital-based nurses”.
2.3Inclusion and exclusion criteria
The inclusion criteria encompassed primary quantitative research that investigates the impact of transformational leadership on job satisfaction and productivity among nurses in healthcare settings. Job satisfaction was defined as “the extent to which employees like their jobs, reflecting their positive or negative feelings towards their work”,[24] while productivity was defined as “the ability of nurses to perform their duties in accordance with hospital standards, ensuring that the work meets the demands of the task with good results”.[25]
The timeframe of January 2016 to March 2024 was selected to capture contemporary healthcare contexts while ensuring sufficient literature availability, encompassing the period following major healthcare system transformations globally (see Table 3). This timeframe ensures inclusion of recently published studies capturing insights following significant shifts in healthcare systems and organizational strategies that may have influenced leadership styles and their outcomes. The scope was restricted to inpatient wards, where nurses often face intricate nursing judgments, endure extended work hours, engage in shift work, and experience high patient turnover.[26]
| Population | Adult nurses in general or specialty areas | Nursing students |
| Setting | Hospital/inpatient wards | Other healthcare settings |
| Keywords | Transformational leadership, job satisfaction, productivity | - |
| Studies | Primary quantitative studies | Literature reviews, qualitative studies |
| Language | English | Other languages |
| Years | January 2016 - March 2024 | Earlier than 2016 |
2.4Study selection and screening
The initial literature search and selection process were conducted independently by the first three researchers. They began by focusing on primary screening criteria and enhanced their search by including peer-reviewed publications from reputable journals and conference proceedings, considering publication dates to ensure relevance. Studies were selected based on predefined eligibility criteria, and a PRISMA flow diagram,[23] was used to refine the search results and display the included articles. The comprehensive literature search was conducted twice to ensure inclusion of all relevant papers, with the final search completed on March 30, 2024, across five databases.
Following the initial selection, search results were imported into Mendeley reference management software (version 1.19.8) to facilitate removal of duplicates. The two researchers then collaborated to compile a list of potentially relevant publications, which was reviewed by two additional researchers (the third and fourth). These reviewers made the final decisions on papers to include in the review, making modifications or exclusions as necessary. After this phase, all selected full-text studies underwent thorough evaluation. Several studies were excluded due to inaccessibility across databases or focus on outcomes outside productivity and job satisfaction. Ultimately, only articles meeting all eligibility criteria were included for further analysis.
2.5Data extraction process
The researchers independently extracted data from the specified studies, capturing details such as authors’ names, publication year, study design, sample characteristics, instruments used, and key findings. Following data extraction, narrative synthesis was conducted, where patterns and recurring categories were systematically identified and categorized across studies. This narrative synthesis allowed for structured comparison of results, highlighting overarching patterns and nuances within the data. To ensure accuracy and consistency, the data extraction and synthesis process was reviewed and verified multiple times.
2.6Quality assessment
The quality of studies was evaluated using the Quality Assessment Tool for Observational Cohort and Cross-Sectional Investigations (Study Quality Assessment Tools | NHLBI, NIH).[27] Each of the 14 questions on the scale has three response options: “yes”, “no”, or “other (cannot determine, not applicable, not reported)”. This instrument assesses the internal validity of a study while taking into account bias. The reviewer assigns a quality rating of ‘good’, ‘fair’, or ‘poor’ to each study after evaluating each criterion.
Researchers independently assessed the studies’ quality. They calculated tertiles of the number of items on the quality scale, as the tool did not provide a straightforward procedure for evaluation. Studies were classified as ‘good quality’ ( 11 ‘yes’ responses, 80%), ‘fair quality’ (7-10 ‘yes’ responses, 50%-79%), or ‘poor quality’ (< 7 ‘yes’ responses, < 50%). All 22 included studies achieved fair quality ratings, with no studies meeting good or poor quality thresholds. Inter-rater agreement was 89% (Cohen’s k = 0.82). All studies were found to be ’fair’ in terms of quality. Any discrepancies in evaluation were resolved through discussion, ensuring consensus was reached.
2.7Data synthesis
Due to heterogeneity in measures and contexts, narrative synthesis was conducted following established guidelines. Effect directions and magnitudes were extracted and synthesized thematically. Following Popay et al. ’s[28] framework, we conducted thematic synthesis by extracting effect directions and magnitudes, identifying patterns across studies, and developing conceptual key patterns to explain transformational leadership mechanisms in nursing contexts.
3.Results
3.1Study selection
Initial database searches yielded 48,590 articles titles, abstracts, and 134 full text were screened resulting in 22 included studies. Using content analysis, after removing duplicates and screening titles and abstracts, 134 articles were identified for further assessment. Five full-text articles were not available, even after contacting the corresponding authors, leaving 129 articles for thorough examination to determine if they met the inclusion criteria. Ultimately, 22 studies were found to meet the criteria for inclusion (see Figure 1 and Table 4).
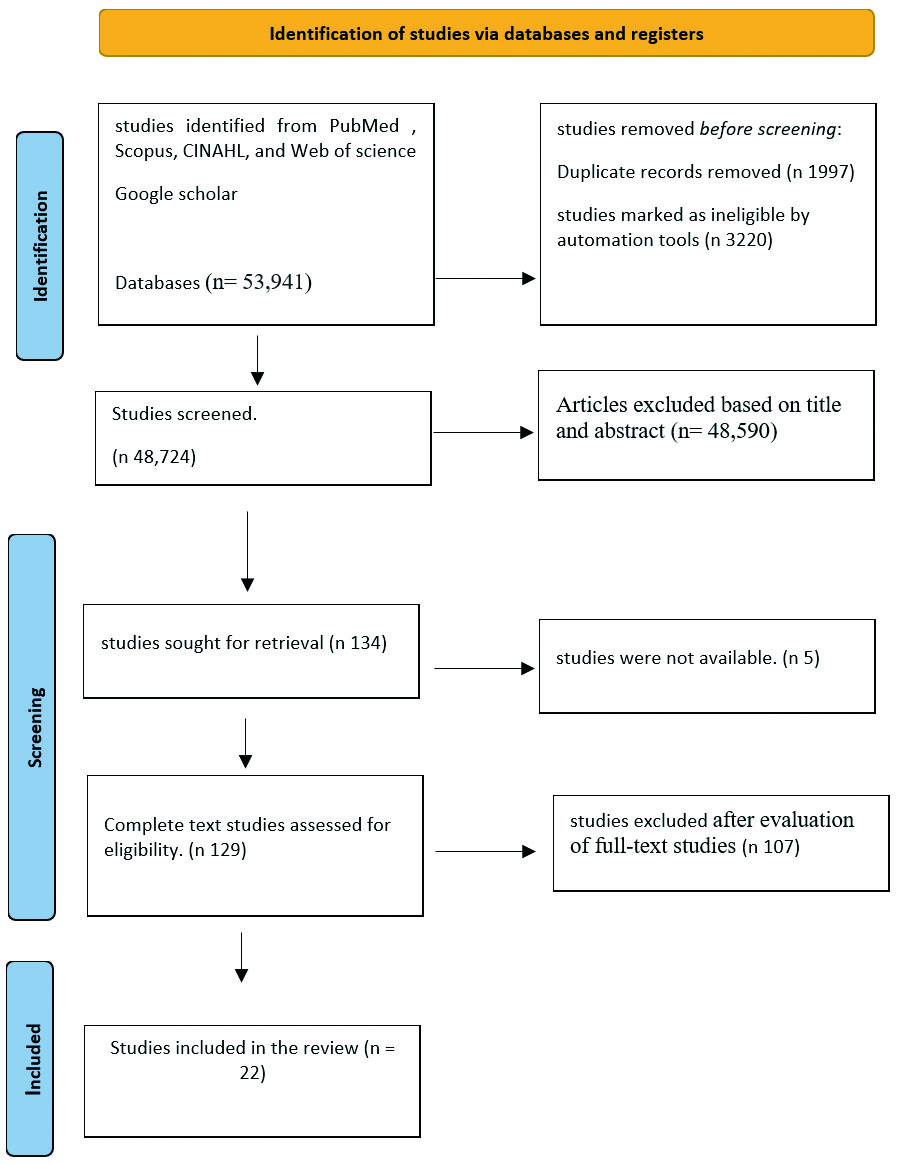
Figure 1.
PRISMA Flow Diagram showing the article selection process[23]
| 1 | Alshahrani and Baig (2016) [ Saudi Arabia |
Cross-sectional. MLQ; Job satisfaction survey. Staff nurses (N = 89) |
Nurses who were employed by transformational leaders reported significantly higher job satisfaction. |
| 2 | Abdelhafiz et al. (2016) [ Jordan |
Cross-sectional. MLQ Staff nurses (N = 200) |
Job satisfaction and the total TL score were positively correlated. The retention of nurses is facilitated by the enhancement of TL practices, which in turn increases their work satisfaction. |
| 3 | Choi et al. (2016) [ Malaysia |
Cross-sectional. MLQ, employee empowerment, and job satisfaction. Staff nurses (N = 200) |
The relationship between TL and nursing staff job satisfaction is mediated by empowerment. |
| 4 | Konstantinou & Prezerakos (2017) [ Greek |
Cross-sectional. MLQ, and the Minnesota Satisfaction Staff nurses (N = 168) |
Indicates that nurses favour a TL style. Satisfaction with internal factors is moderate, while satisfaction with extrinsic factors is low. |
| 5 | Khanzada et al. )2018) [ Pakistan |
Cross-sectional. The researchers used structural equation modeling to test their hypothesized model. Staff nurses (N = 358) |
TL has a substantial impact on the improvement of empowering workstations, the increase in nurse job satisfaction, and the reduction of adverse patient outcomes. |
| 6 | Manesh et al. (2018) [ Malaysia |
The questionnaire consists of Nurses’ attitudes, subjective norms, and perceived behavioral control. Staff nurses (N = 135) |
Demonstrates a robust positive correlation between the four characteristics of TL and work performance. |
| 7 | Naseem et al. (2018) [ Pakistan |
Cross-sectional. MLQ, and the Minnesota Satisfaction Questionnaire (MSQ). Staff nurses (N = 211) |
The nursing staff expressed a higher level of satisfaction with transformative leadership, which in turn resulted in increased job satisfaction, improved performance, and productivity among nurses. |
| 8 | Alloubani et al. (2019) [ Jordan |
Cross-sectional. MLQ and the patient satisfaction with nursing care quality questionnaire. Staff nurses (50 nurse managers, 150 staff nurses) |
The TL style was significantly positively associated with improved job satisfaction, leadership efficacy, overall nursing care quality, and employee effort. |
| 9 | Albagawi (2019) [ Saudi Arabia |
Cross-sectional. MLQ, and the work quality index Staff nurses (N = 184) |
TL is linked to higher job satisfaction, |
| 10 | Asif et al. (2019) [ Pakistan |
Cross-sectional. Transformational leadership, Structural empowerment, Job satisfaction, Adverse patient outcomes, Quality of care Staff nurses (N = 600) |
Job satisfaction is significantly correlated with TL. TL, structural empowerment, job satisfaction, and unfavourable patient outcomes are all associated with the quality of care that nurses evaluate. |
| 11 | Jatianita et al. (2020) [ Indonesia |
Cross-sectional. Nurse Productivity, Transformational Leadership Style, and Achievement Motivation And intervening by competency Development activity. Staff nurses (N = 45) |
TL and motivation have an impact on the development of competence and nursing productivity, with appropriate growth enhancing nurse productivity. |
| 12 | Lai et al. (2020) [ Taiwan |
Cross-sectional. Transformational leadership scale Work engagement scale Task performance scale. A helping behaviors scale was used. Staff nurses (N = 507) |
The positive correlation between TL, job performance, and assisting behavior is influenced by work engagement. |
| 13 | Ullah (2020) [ Pakistan |
Cross-sectional. Transformational Leadership Style, performance outcomes measures. Staff nurses (N =206) |
Job satisfaction of staff nurses is positively correlated with TL. |
| 14 | ALFadhalah & Elamir (2021) [ Kuwait |
Cross-sectional. Multifactor Leadership Questionnaire and the Organizational Description Questionnaire. Staff nurses (N = 192) |
TL positively impacts the organization's care quality. |
| 15 | Wang et al. (2021) [ Taiwan |
Mixed-method explanatory sequential study. Staff nurses (N = 73 nurse managers and 719 nurses.) |
During the quantitative phase, TL style is positively correlated with improved nurses’ job performance |
| 16 | Uslu Sahan & Terzioglu (2022) [ Turkey |
Cross-sectional. leaders Commitment inventory (self/observer), organizational commitment scale, and job satisfaction scale. Staff nurses (N = 153 nurses) |
The TL practices of nurse administrators were more favourable for staff nurses. The job satisfaction of staff nurses was influenced by the TL style. |
| 17 | Abdullah Alrasheedi et al. (2022) [ Saudi Arabia |
Cross-sectional. MLQ, and the Job Satisfaction Survey. Staff nurses (N = 437) |
TL style was more effective for predicting job satisfaction. |
| 18 | Aly et al. (2022) [ Saudi Arabia |
Cross-sectional. MLQ, and Nurses Knowledge and Skills Staff nurses (N = 47) |
TL styles enhance the productivity of staff nurses in the areas of communication, personnel and professional development, health safety, security, quality, equality, and diversity. |
| 19 | Othman & Khrais (2022) [ Jordan |
Cross-sectional. Global Transformational Leadership (GTL) scale, a job satisfaction survey Staff nurses (N = 253) |
The relationship between job satisfaction and TL is notably positive. It is possible for TL to assist nurses in enhancing their job satisfaction and organizational commitment. |
| 20 | Gashaye et al. (2023) [ Ethiopia |
Cross-sectional. MLQ, and job satisfaction Staff nurses (N = 403) |
TL is a critical style for nurse leaders to employ in order to achieve organizational objectives and enhance the productivity of their staff. |
| 21 | Mughal (2023) [ Saudi Arabia |
Cross-sectional. MLQ, Behavioral trust scale and nurse’s performance. Staff nurses (N = 100) |
Trust is partially mediated by the TL, that influence behavior attributes and the performance of nurses. Retaining a productive nursing workforce is significantly facilitated by trusted leaders. |
| 22 | Ismael et al. (2024) [ Egypt |
Cross-sectional. MLQ and McCloskey/Mueller Satisfaction Scale. Staff nurses (N = 248) |
There is a highly statistically significant positive correlation between job satisfaction and TL style among nurses. |
3.2Quality assessment
All studies achieved fair quality ratings, with consistent weaknesses in confounder control and sampling representativeness (see Table 5).
| Study objectives clearly stated | 22 (100) | 0 (0) | 0 (0) |
| Population clearly defined | 18 (81.8) | 4 (18.2) | 0 (0) |
| Exposure assessed consistently | 15 (68.2) | 7 (31.8) | 0 (0) |
| Outcome measures valid/reliable | 16 (72.7) | 6 (27.3) | 0 (0) |
| Confounders addressed | 5 (22.7) | 12 (54.5) | 5 (22.7) |
| Overall Quality Rating | 0 (0) | 22 (100) | 0 (0) |
3.3Quantitative synthesis
The findings revealed a strong association between transformational leadership style and job satisfaction among nurses, ultimately leading to improved performance and productivity. Specifically, seventeen studies reported a statistically significant positive correlation, while five studies demonstrated that transformational leadership style promotes job satisfaction among nurses (see Table 6).
| Job Satisfaction | 20 | 17 (85.0%) | 0.43-0.944 | Strong positive association |
| Productivity/Performance | 15 | 13 (86.7%) | 0.35-0.78 | Consistent productivity enhancement |
| Organizational Commitment | 8 | 7 (87.5%) | 0.41-0.69 | High correlation with TL |
| Work Engagement | 6 | 6 (100%) | 0.48-0.73 | Universal positive effects |
3.4Regional and cultural analysis
Table 7 summarizes the regional distribution of included studies and their average correlation coefficients between transformational leadership (TL) and job satisfaction. The highest mean correlation was observed in Middle Eastern countries (r = 0.71), suggesting that TL may be particularly effective in hierarchical and collectivist cultures where leaders are expected to provide vision and support. In contrast, regions such as South Asia and East Asia showed slightly lower, yet still strong, correlations (r = 0.63 and r = 0.65, respectively), often mediated by empowerment and professional development. The “Other” category, which includes diverse healthcare contexts, also demonstrated consistent positive associations, albeit with more variation. These findings highlight that while TL is broadly effective across cultures, the mechanisms and magnitude of its influence may differ based on organizational norms and societal values.
| Middle East (Saudi Arabia, Jordan, Kuwait) | 9 | Public/Mixed | 0.71 | Highest correlations observed; hierarchical leadership cultures likely amplify TL impact on staff morale. Strong emphasis on respect for authority and collectivism. |
| South Asia (Pakistan) | 4 | Mixed/Private | 0.63 | TL linked to satisfaction via empowerment and reduced turnover, though less institutional leadership training noted. |
| East Asia (Malaysia, Taiwan) | 4 | Public/Insurance | 0.65 | Empowerment and professional development emerged as key mediators; TL effects moderated by organizational structure. |
| Other (Indonesia, Egypt, Turkey, Greece, Ethiopia) | 5 | Various | 0.58 | Consistent positive effects despite varied healthcare models. Cultural differences may limit TL expression, but outcomes remain favorable. |
3.5Pattern analysis
This section summarizes the key patterns identified across the reviewed studies. Three primary patterns emerged from the synthesis:
Transformational leadership has been shown to have a significant positive effect on job satisfaction. Studies have reported correlation coefficients ranging from moderate to strong, indicating a robust relationship between these variables. For instance, Asif et al. found a correlation coefficient of 0.43, while another study reported a coefficient of 0.944, both suggesting a strong positive relationship between transformational leadership and job satisfaction.[11, 36, 46]
The role of transformational leadership in influencing job satisfaction is widely supported in the literature, with the majority of studies reporting a positive correlation between transformational leadership and job satisfaction. Specifically, the majority found a positive association between transformational leadership and job satisfaction, highlighting that transformational leadership fosters a supportive and empowering work environment that enhances creativity, engagement, and personal commitment among nurses.[11, 25, 30, 34, 42, 47] However, a minority of studies found either a weak positive correlation, suggesting that in some contexts, transformational leadership alone may not be sufficient to significantly impact job satisfaction without other supporting factors in place.[17, 30, 40]
Other factors such as the work environment, structural empowerment, and individual/contextual elements also play significant roles in job satisfaction among nurses. Positive correlations were noted between job satisfaction and elements of the work environment, including balanced workloads, pace, and professional development opportunities.[16, 31, 37, 48] Structural empowerment, which provides nurses with resources and decision-making authority, is highly correlated with job satisfaction, as it enhances their ability to meet patient needs effectively.[31]
The relationships between transformational leadership, achievement motivation, and nurse productivity are predominantly positive.[6, 18, 25] Transformational leadership positively impacts productivity by fostering a work culture that values competence, motivation, and satisfaction.[25, 33, 49] Achievement motivation, when supported by a transformational leadership style, also has a positive influence on productivity, as it encourages nurses to seek continuous development and high performance.[25]
There is considerable consistency in the literature supporting a positive association between transformational leadership and nurse productivity. Multiple studies[6, 18, 50, 51] have reported that transformational leadership enhances productivity by positively influencing motivation and competency development. Aly et al.,[6] emphasize the role of transformational leadership in fostering a motivated and capable nursing staff, resulting in improved productivity and patient outcomes.
While demographic factors (such as age, experience, education level) also influence productivity, their effects are less consistent across studies.[52] Some studies suggest that more experienced or highly educated nurses may respond more positively to transformational leadership,[6] showing higher productivity levels, while others indicate that transformational leadership impacts productivity consistently across different demographic groups.
The correlation between transformational leadership and job satisfaction is well-supported in the literature. Studies indicate that transformational leadership is positively associated with job satisfaction, particularly among healthcare professionals,[40] where leadership styles significantly impact staff morale and engagement.[7, 35] Research demonstrates that transformational leadership fosters a nurturing environment for nurses,[33] resulting in increased satisfaction by promoting a sense of purpose and commitment within their roles.
In addition to job satisfaction, transformational leadership is also positively correlated with productivity. Empirical evidence shows that transformational leadership enhances productivity by improving communication, promoting staff development, and creating a positive work environment.[53] Studies have found that transformational leadership fosters productivity among nurses by encouraging a collaborative atmosphere and enhancing skills through people development and open communication.[25]
4Discussion
This systematic review provides robust evidence for positive associations between transformational leadership and nursing outcomes across diverse international contexts. The consistency of findings across 22 studies from 11 countries strengthens confidence in the generalizability of transformational leadership benefits. Transformational leadership has consistently been shown to have a positive impact on the job satisfaction of nurses in a variety of studies.[12, 35, 42, 45, 48, 54, 55, 56] Research has shown that staff nurses experience higher levels of job satisfaction when working under transformational leadership styles.[17, 37, 57]
Additionally, research indicates that transformational leadership is the most significant factor in the improvement of human resources productivity in teaching hospitals.[52]
4.1Cultural and contextual considerations
Regional variations in effect sizes suggest cultural moderation of transformational leadership effectiveness, with implications for global healthcare leadership development. Hierarchical healthcare systems in Middle Eastern contexts showed stronger correlations (mean r = 0.71), potentially reflecting cultural values that emphasize respect for authority and inspirational leadership. In contrast, more egalitarian healthcare systems demonstrated moderate but consistent effects (mean r = 0.58-0.65), suggesting universal applicability with cultural adaptation requirements. Nurses generally perceive their leaders as engaging in transformational behaviors, as indicated by research conducted in a variety of countries.[4, 51, 58] This finding has important implications for global healthcare organizations implementing leadership development programs.
4.2Pathway of action
Our analysis identified four primary pathways through which transformational leadership enhances nursing outcomes see Figure 2:
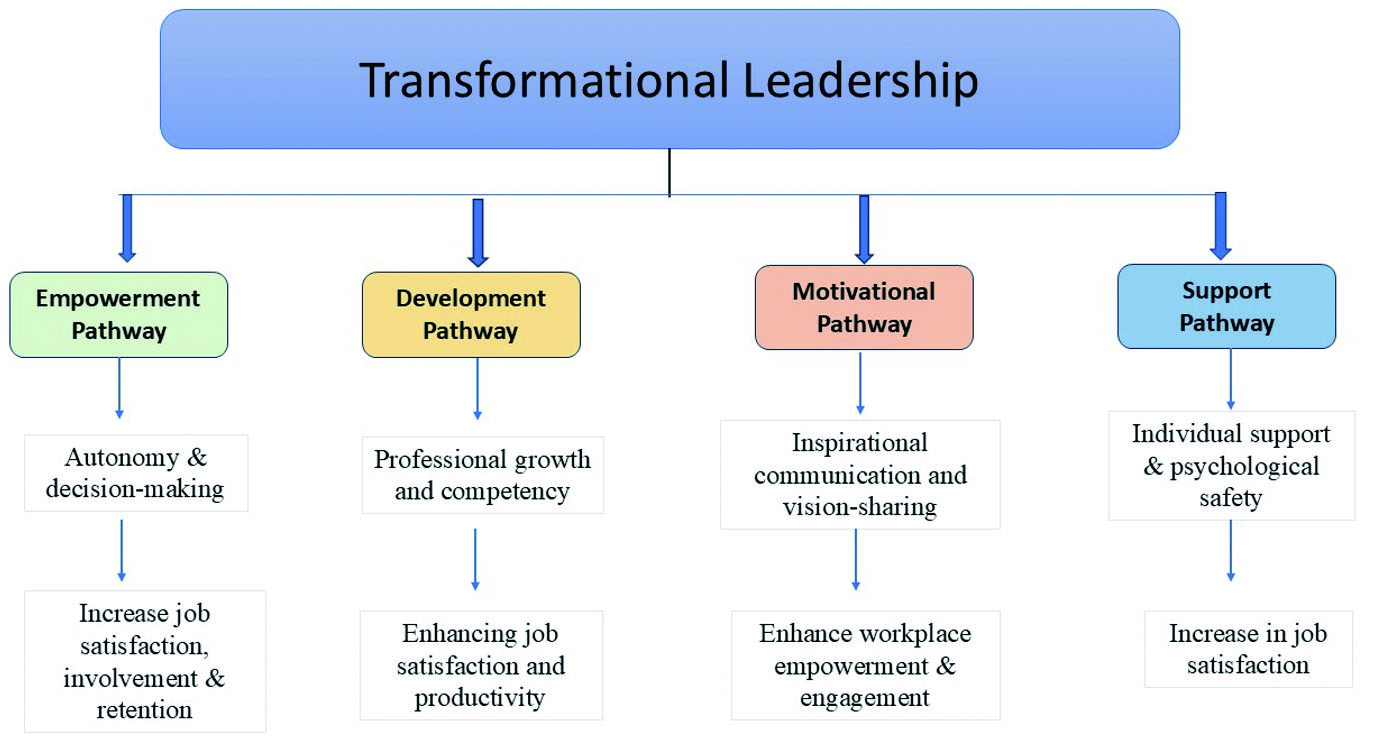
Figure 2.
Conceptual framework: Pathways linking transformational leadership to nurse job satisfaction and productivity
4.3Limitations
Several limitations warrant consideration. The sole emphasis on quantitative studies, albeit ensuring methodological consistency, overlooked potentially useful insights from qualitative research that may elucidate processes and contextual elements. Secondly, all research considered used cross-sectional designs, which exclude causal conclusions about the impacts of transformative leadership. Third, healthcare companies often use many leadership styles concurrently, and our emphasis on transformational leadership alone may not encompass the intricacies of actual leadership dynamics. Fourth, publication bias may exaggerate effect sizes, since research with non-significant results are less often reported. The investigation of culture was restricted by insufficient cultural data in primary research, hindering a more profound exploration of cultural mediators. Moreover, our inquiry was confined to English-language publications, which may have omitted pertinent research from non-English speaking nations, hence possibly constraining the multicultural viewpoint we sought to attain in analyzing global healthcare environments Additionally, no eligible studies from North America were included in this review. This may limit the generalizability of findings to Western healthcare systems and highlights a need for future reviews to synthesize findings from North American contexts using comparable quantitative criteria. Finally, heterogeneity in measurement instruments prevented meta-analysis.
5Conclusions
This review emphasizes the consistent advantages of transformational leadership within global healthcare systems, underscoring its significance in enhancing nursing job satisfaction and productivity. The findings support existing evidence and highlight the necessity for context-sensitive implementation of leadership practices.
Future research should investigate the integration of transformational leadership training within nursing education programs and evaluate its effectiveness in preparing prospective nurse leaders. The impact of ongoing professional development in healthcare organizations, including mentorship programs, structured leadership pathways, and organizational culture, warrants examination to assess their influence on sustaining transformational leadership behaviors in clinical practice. Longitudinal studies are necessary to identify the causal relationships among leadership styles, staff satisfaction, and patient outcomes, especially in resource-constrained and dynamically changing healthcare environments.
Clinical and Policy Implications: Healthcare organizations should immediately implement evidence-based transformational leadership development programs. Hospital managers and administrators can implement transformational leadership as an effective strategy to boost nursing work satisfaction, emphasizing innovation and fostering meaningful interactions between nurse managers and staff to improve supervision and align with organizational goals.[40] A clear vision, well-defined objectives, and the empowerment of nurses contribute to better job satisfaction and develop nurse managers who lead by example, instilling trust and confidence among their subordinates. Nurse leaders should develop mechanisms to oversee, analyze, resolve, and evaluate nurses’ tasks and work environments while fostering open and cooperative engagement with their teams.
Implementation Recommendations: Requirement of leadership development in healthcare accreditation standards, emphasizing transformational leadership principles - Investment in organizational leadership development infrastructure at institutional and system levels - Policy mandates for evidence-based leadership training in healthcare institutions - Integration of transformational leadership principles in nursing education curricula - Development of standardized competency frameworks for nurse leadership roles
Authors contributions
S.A.H., and Z.A.A. were responsible for study design and revising. Z.A.H., S.A.A., and R.M.B. were responsible for data collection. S.A.H, and R.M.B. drafted the manuscript and S.A.H., and Z.A.A revised it. All authors read and approved the final manuscript. In this paragraph, also explain any special agreements concerning authorship, such as if authors contributed equally to the study.
Funding
The study did not get any financial support from external sources.
Conflicts of Interest Disclosure
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Informed consent
Obtained.
Ethics approval
The Publication Ethics Committee of the Association for Health Sciences and Education. The journal’s policies adhere to the Core Practices established by the Committee on Publication Ethics (COPE).
Provenance and peer review
Not commissioned; externally double-blind peer reviewed.
Data availability statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Data sharing statement
No additional data are available.
Acknowledgements
We greatly appreciate the valuable contributions of colleagues who assisted in conducting the study, every team member who took the time to participate in this study, and critiquing the manuscript.
References
- Kamalasanan A, Subbarayalu A, MR A. Nurses’ perception on the quality of healthcare services: A cross-sectional study. Int J Healthc Manag. 2023;17(4):817-826. doi:10.1080/20479700.2023.2246241
- Goh A, Ang S, Della P. Leadership style of nurse managers as perceived by registered nurses: A cross-sectional survey. Proceedings of Singapore Healthcare. 2018;3(27):205-210. doi:10.1177/2010105817751742
- Saleh U, Profile S, Alsubhi H. The impact of nurse managers’ leadership styles on ward staff. BNJ. 2018;27(4):197-203. PMID:29457941 doi:10.12968/bjon.2018.27.4.197
- Olu-Abiodun O, Abiodun O. Perception of transformational leadership behaviour among general hospital nurses in Ogun State, Nigeria. Int J Africa Nurs Sci. 2017;6:22-27. doi:10.1016/j.ijans.2017.02.001
- Abd-Elrhaman E, Abd-Allah N. Transformational Leadership Educational Program for Head Nurses and its Effect on Nurses’ Job Performance. Am J Nurs Sci. 2018;7(4):127-136. doi:10.11648/j.ajns.20180704.13
- Aly S, Alghabbashi M, Alhusyeni N. The association of leadership styles and empowerment with nurses’ organizational commitment in an acute health care setting: a cross-sectional study. BMC Nurs. 2016;15:38. PMID:27293380 doi:10.1186/s12912-016-0161-7
- Ullah Z, Khan M. The impact of transactional and transformational leadership on job related outcomes in the nursing profession. Sarhad J. Manag. Sci. 2020;6(1):143-159.
- Bass B, Avolio B. Transformational leadership and organizational culture. Public Adm Q. 1993;17(1):112-121.
- Bass B, Avolio B, Atwater L. The Transformational and Transactional Leadership of Men and Women. Appl Psychol. 1996;45(1):5-34. doi:10.1111/j.1464-0597.1996.tb00847.x
- Shobe K. Productivity driven by job satisfaction, physical work environment, management support and job autonomy. Bus Econ J. 2018;9(2):1-9.
- Abdelhafiz I, Alloubani A, Almatari M. Impact of leadership styles adopted by head nurses on job satisfaction: a comparative study between governmental and private hospitals in Jordan. J Nurs Manag. 2016;24(3):384-392. PMID:26310389 doi:10.1111/jonm.12333
- Alloubani A, Akhu-Zaheya L, Abdelhafiz I. Leadership Styles’ Influence on the Quality of Nursing Care. Int J Health Care Qual Assur. 2019;32(6):1022-1033. PMID:31282258 doi:10.1108/ijhcqa-06-2018-0138
- Ferreira V, Amestoy S, Silva G. Transformational leadership in nursing practice: challenges and strategies. SciELO Bras. 2020;73(6):e20190364. PMID:32785519 doi:10.1590/0034-7167-2019-0364
- Ibrahim A, El-Monshed A, El-Sehrawy M. Enhancing Nurses’ Well-Being: Exploring the Relationship between Transformational Leadership, Organizational Justice, and Quality of Nursing Work Life. J Nurs Manag. 2023. PMID:40225606 doi:10.1155/2023/2337975
- Iqbal K, Fatima T, Naveed M. The Impact of Transformational Leadership on Nurses’ Organizational Commitment: A Multiple Mediation Model. Eur J Investig Heal Psychol Educ. 2020;10(1):262-275. PMID:34542484 doi:10.3390/ejihpe10010021
- Ystaas L, Nikitara M, Ghobrial S. The Impact of Transformational Leadership in the Nursing Work Environment and Patients’ Outcomes: A Systematic Review. Nurs Reports. 2023;13(3):1271-1290. PMID:37755351 doi:10.3390/nursrep13030108
- Alshahrani F, Baig L. Effect of Leadership Styles on Job Satisfaction Among Critical Care Nurses in Aseer, Saudi Arabia. J Coll Physicians Surg Pak. 2016;26(5):366-370.
- Aly S, Alghabbashi M, Alhusyeni N. The Relationship between the new Leadership Styles and Nursing Productivity. Pakistan J Med Heal Sci. 2022;16(5):836-841. doi:10.53350/pjmhs22165836
- Sabbah I, Ibrahim T, Khamis R. The association of leadership styles and nurses well-being: A cross-sectional study in healthcare settings. Pan Afr Med J. 2020;36:1-14. PMID:33193982 doi:10.11604/pamj.2020.36.328.19720
- Alghamdi R, Albloushi M, Alzahrani E. Nursing Education Challenges from Saudi Nurse Educators’ and Leaders’ Perspectives: A Qualitative Descriptive Study. Int J Nurs Educ Scholarsh. 2019. PMID:30798324 doi:10.1515/ijnes-2018-0027
- Al-Yateem R, Almarzouqi A, Dias J, et al.. Nursing in the United Arab Emirates: current challenges and opportunities. J Nurs Manag. 2020. PMID:32100891 doi:10.1111/jonm.12984
- Nashwan A, Hashish E, Cureus A. Exploring the National Nursing Research Priorities in the Eastern Mediterranean Region and Overcoming the Associated Challenges: An Expert Opinion. Cureus. 2024;16(7):e64540. doi:10.7759/cureus.64540
- Page M, Mckenzie J, Bossuyt P. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev. 2021;10:89. PMID:33781348 doi:10.1186/s13643-021-01626-4
- Kvist T, Mäntynen R, Vehviläinen-Julkunen K. Does Finnish hospital staff job satisfaction vary across occupational groups? BMC Health Serv Res. 2013;13:376. PMID:24088218 doi:10.1186/1472-6963-13-376
- Jatianita L, Wekadigunawan None, Aida M. Transformational leaders can improve Achievement Motivation and Competence Development to support. Nurses Productivity. 2020.
- Hayes L, O’Brien-Pallas L, Duffield C. Nurse turnover: A literature review – An update. Int J Nurs Stud. 2012;49(7):887-905. PMID:22019402 doi:10.1016/j.ijnurstu.2011.10.001
- Study Quality Assessment Tools|NHLBI, NIH. 2014. https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools
- Popay J, Roberts H, Sowden A. Guidance on the conduct of narrative synthesis in systematic reviews. A Prod from ESRC methods Program Version 1: b92. 2006.
- Choi S, Goh C, Adam M. Transformational leadership, empowerment, and job satisfaction: The mediating role of employee empowerment. Hum Resour Health. 2016;14:1-14. PMID:27903294 doi:10.1186/s12960-016-0171-2
- Konstantinou C, Prezerakos P. Relationship Between Nurse Managers’ Leadership Styles and Staff Nurses’ Job Satisfaction in a Greek NHS Hospital. Am J Nurs Sci. 2017;7(3):45-50.
- Khanzada B, Naeem S, Butt H. Impact of Transformational Leadership on Job Satisfaction and Patient Safety Outcomes in Health Sector of Pakistan. J Heal Educ Res Dev. 2018. doi:10.4172/2380-5439.1000251
- Manesh M, Singh J, Hussain I. Transformational Leadership and Contextual Performance: A Quantitative Study among Nursing Staff in Kuala Lumpur. Int J Manag Sustain. 2018;7(2):101-112. doi:10.18488/journal.11.2018.72.101.112
- Naseem S, Afzal M, Sehar S. Relationship between Leadership Styles of Nurse Managers and Staff Nurses Job Satisfaction in Public Hospital of Punjab, Pakistan. Int J Soc Sci Manag. 2018;5(3):201-208. doi:10.3126/ijssm.v5i3.20611
- Alloubani A, Akhu-Zaheya L, Abdelhafiz I. Leadership styles’ influence on the quality of nursing care. Int J Health Care Qual Assur. 2019;32(6):1022-1033. PMID:31282258 doi:10.1108/IJHCQA-06-2018-0138
- Albagawi B. Leadership Styles of Nurse Managers and Job Satisfaction of Staff Nurses: Correlational Design Study. Eur Sci J ESJ. 2019;15(3):254-275. doi:10.19044/esj.2019.v15n3p254
- Asif M, Jameel A, Hussain A. Linking Transformational Leadership with Nurse-Assessed Adverse Patient Outcomes and the Quality of Care: Assessing the Role of Job Satisfaction and Structural Empowerment. Int J Environ Res Public Health. 2019;16(3):2381. PMID:31277478 doi:10.3390/ijerph16132381
- Lai F, Tang H, Lu S. Transformational Leadership and Job Performance: The Mediating Role of Work Engagement. SAGE Open. 2020. doi:10.1177/2158244019899085
- ALFadhalah T, Elamir H. Organizational Culture, Quality of Care and Leadership Style in Government General Hospitals in Kuwait: A Multimethod Study. J Healthc Leadersh. 2021. PMID:34703349 doi:10.2147/JHL.S333933
- Wang H, Chen Y, Yang F. Relationship between transformational leadership and nurses’ job performance: The mediating effect of psychological safety. Soc Behav Pers. 2021. doi:10.2224/sbp.9712
- Uslu SF, Terzioglu F. Transformational leadership practices of nurse managers: the effects on the organizational commitment and job satisfaction of staff nurses. Leadersh Health Serv (Bradf Engl). 2022. PMID:35612396 doi:10.1108/LHS-11-2021-0091
- Abdullah Alrasheedi M, Moteb Alrashaidi F, Abdel Hameed Shahin M. Leadership Styles and Job Satisfaction among Nurses of Medical-Surgical Floors in Governmental Hospitals in Qassim Region, Saudi Arabia. Int J Med Res Heal Sci. 2022;11:50-63.
- Othman T, Khrais H. The relationship between transformational leadership, job satisfaction, and organizational commitment in Jordanian nurses. Anaesthesia, Pain Intensive Care. 2022;26(3):304-309. doi:10.35975/apic.v26i3.1896
- Gashaye M, Beyene D, Belay A. Perceived Utilization of Leadership Styles Among Nurses. Risk Manag Healthc Policy. 2023;16:215-224. PMID:36819844 doi:10.2147/rmhp.s388966
- Mughal Y. Mediating Role of Trust in Linking Transformational Leadership Style and Nurses’ Performance. Gomal Univ J Res. 2023;39(3):266-276. doi:10.51380/gujr-39-03-02
- Ismael H, Sleem W, Abd el-Ghani A. Relationship Between Transformational Leadership Style and Job Satisfaction among Nurse. Mansoura Nurs J. 2024;11:357-368. doi:10.21608/mnj.2024.350482
- Wijayanti K, Aini Q. The Influence of Transformational Leadership Style to Nurse Job Satisfaction and Performance in Hospital. J World Sci. 2022;1(7):485-499. doi:10.58344/jws.v1i7.69
- Wijayanti K, Schütze H, MacPhail C. Parents’ attitudes, beliefs and uptake of the school-based human papillomavirus (HPV) vaccination program in Jakarta, Indonesia – A quantitative study. Prev Med Reports. 2021. PMID:34976699 doi:10.1016/j.pmedr.2021.101651
- Hasan A, Ahmad S, Osman A. Transformational leadership and work engagement as mediators on nurses’ job performance in healthcare clinics: work environment as a moderator. Leadersh Heal Serv. 2023;36(4):537-561. PMID:37093237 doi:10.1108/LHS-10-2022-0097
- Dorji T, Nopsopon T, Tamang S. Human papillomavirus vaccination uptake in low-and middle-income countries: a meta-analysis. ECLINICALMEDICINE. 2021. PMID:33997733 doi:10.1016/j.eclinm.2021.100836
- Jatianita L, Wekadigunawan W, Aida M. Transformational leaders can improve Achievement Motivation and Competence Development to support Nurses Productivity. Journal of Multidisciplinary Academic. 2020;4(6):407-411.
- ALFadhalah T, Elamir H. Organizational Culture, Quality of Care and Leadership Style in Government General Hospitals in Kuwait: A Multimethod Study. J Healthc Leadersh. 2021;13:243-254. PMID:34703349 doi:10.2147/JHL.S333933
- Vatankhah S, Alirezaei S, Khosravizadeh O. Role of transformational leadership on employee productivity of teaching hospitals: using structural equation modeling. Electron Physician. 2017;9(8):4978-4984. PMID:28979731 doi:10.19082/4978
- Alzahrani S, Hasan A. Transformational Leadership Style on Nursing Job Satisfaction Amongst Nurses in Hospital Settings: Findings From Systematic Review. Glob J Health Sci. 2021;11(6):50-63. doi:10.5539/gjhs.v11n6p25
- Asif M, Jameel A, Hussain A. Linking Transformational Leadership with Nurse-Assessed Adverse Patient Outcomes and the Quality of Care: Assessing the Role of Job Satisfaction and Structural Empowerment. Int J Environ Res Public Health. 2019;16(13):2381. PMID:31277478 doi:10.3390/ijerph16132381
- Boamah S, Spence Laschinger H, Wong C. Effect of transformational leadership on job satisfaction and patient safety outcomes. Nurs Outlook. 2018;66(2):180-189. PMID:29174629 doi:10.1016/j.outlook.2017.10.004
- Wijayanti K, Aini Q. The Influence of Transformational Leadership Style to Nurse Job Satisfaction and Performance in Hospital. J World Sci. 2022;1(7):485-499. doi:10.58344/jws.v1i7.69
- Gashaye M, Tilahun D, Belay A. Perceived Utilization of Leadership Styles Among Nurses. Risk Manag Healthc Policy. 2023;16:215-224. PMID:36819844 doi:10.2147/RMHP.S388966
- Morsiani G, Bagnasco A, Sasso L. How staff nurses perceive the impact of nurse managers’ leadership style in terms of job satisfaction: a mixed method study. J Nurs Manag. 2017;25:119-128. PMID:27917561 doi:10.1111/jonm.12448
- Choi S, Fei G, Hisyam Adam M. Transformational Leadership, Empowerment, and Job Satisfaction: The Mediating Role of Employee Empowerment. Hum Resour Health. 2016. PMID:27903294 doi:10.1186/s12960-016-0171-2
- Asiri S, Rohrer W, Al-Surimi K. The association of leadership styles and empowerment with nurses’ organizational commitment in an acute health care setting: a cross-sectional study. BMC Nurs. 2016;15:38. PMID:27293380 doi:10.1186/s12912-016-0161-7


